Last Reviewed: 01 Apr 2026
Bulimia Nervosa is a type of eating disorder characterised by episodes of binge eating followed by compensatory behaviours, which are intended to prevent weight gain. The term binge is commonly misused to describe mild overeating, or even normal eating. In reality, during a binge episode a person will eat an unusually large amount of food in a short period of time. People with Bulimia Nervosa experience a sense of loss of control during a binge eating episode and then engage in compensatory behaviours because of intense feelings of guilt and shame.
Compensatory behaviours are intended to prevent weight gain after binge eating. They include self-inducing vomiting, dieting, fasting, excessive exercise and the misuse of laxatives, diuretics or other medications and drugs. Often individuals can get stuck in a cycle of bingeing and purging.
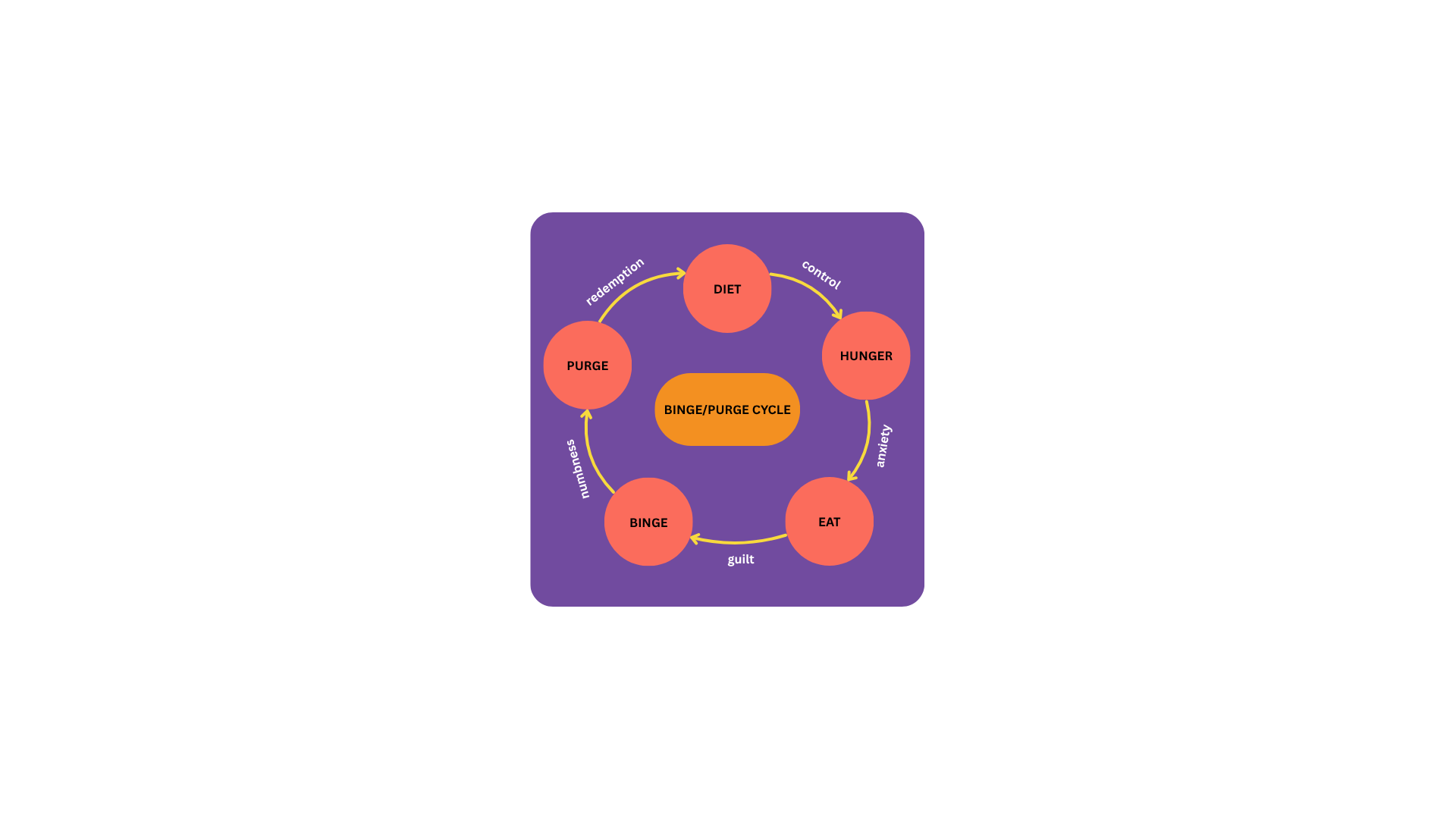
Anyone experiencing this pattern of eating should seek treatment as it can be resolved.
Bulimia Nervosa is a serious mental illness that has significant mental health impacts and a range of physical complications, some of which can be life threatening. People who experience Bulimia Nervosa often keep their behaviours a secret, due to extreme levels of guilt and shame, which gets in the way of seeking help. In addition, many health professionals (and others) have very stereotyped ideas of what someone with an eating disorder 'looks' like, so people who are not severely underweight are frequently overlooked in health care settings, and when they do ask for help, their experience can be minimised or dismissed. This type of stigma and stereotyping can make it hard for people who experience bulimia nervosa and other eating disorders to access the treatment that they need and deserve.
Bulimia Nervosa is often used as a way of dealing with underlying personal, emotional, and psychological difficulties. It can be experienced by the individual as helping them to cope by numbing their emotions, providing a distraction or a sense of accomplishment, and thereby helping them feel in control.
The exact causes of Bulimia Nervosa are not known. A range of factors can play a role in the development of the disease, including genetics, environment, and societal influences as well as trauma history, perfectionism, pre-existing anxiety or depression. Bulimia Nervosa generally develops in the late teens and is experienced by men as well as women. People with Bulimia Nervosa place extreme importance on their body shape and weight in determining their self-worth.
Bulimia Nervosa is a treatable illness and there is a lot of evidence about the treatments that work. The sooner someone gets help, the better
Up to 3.8% of Australians will experience Bulimia Nervosa in their lifetime.
Frequent changes in weight
Signs of damage due to vomiting, including swelling around the cheeks or jaw, calluses on knuckles, damage to teeth and bad breath
Feeling bloated and constipated
Disturbance of menstrual periods in women
Fainting or dizziness
Feeling tired and not sleeping well
Preoccupation with eating, food, body shape and weight
Sensitivity to comments relating to food, weight, body shape or exercise
Low self-esteem and feelings of self-loathing, shame or guilt, particularly after eating
Distorted body image
Obsession with food and need for control
Depression, anxiety, or irritability
Body dissatisfaction
Evidence of eating large amounts of food
Vomiting or using laxatives, enemas, appetite suppressants or diuretics
Eating in private and avoiding meals with other people
Anti-social behaviour, spending more and more time alone
Repetitive or obsessive behaviours relating to body shape and weight
Secretive behaviour around food
Dieting Behaviour
Erratic Behaviour
Self-harm, substance abuse or suicide attempt
Research suggests that a range of psychological therapies such as Cognitive Behaviour Therapy (CBT), Dialectical Behaviour Therapy (DBT) and Interpersonal Therapy (IPT) are most effective. Ongoing medical monitoring by a GP and nutrition support with a Dietitian is also important.
For adults, CBT has been shown to be the most effective for treatment of Bulimia Nervosa. ‘Guided Self-help’ has also been shown to be effective. For children and adolescents, both Family Based Treatment (FBT) and CBT have research to support their use with Bulimia Nervosa.
Hospital-based treatment may be required if the symptoms are very severe or if there are any medical complications that need immediate treatment. A trained and skilled community clinician will almost always be needed to deliver evidence-based treatment
For anyone with Bulimia Nervosa, it is important to seek care from an empathetic and skilled GP who can remain involved throughout treatment.
References
American Psychiatric Association. (2022). Diagnostic and statistical manual of mental disorders (5th ed. Text Revision). Washington, DC: American Psychiatric Press.
Bagaric M, Touyz S, Heriseanu A, Conti J, Hay P. Are bulimia nervosa and binge eating disorder increasing? Results of a population-based study of lifetime prevalence and lifetime prevalence by age in South Australia. European Eating Disorders Review. 2020;28(3):260-268. doi:10.1002/erv.2726
Barakat, S., McLean, S. A., Bryant, E., Le, A., Marks, P., Touyz, S., & Maguire, S. (2018). Risk factors for eating disorders: findings from a rapid review. Journal of Eating Disorders. doi: 10.1186/s40337-022-00717-4
Kehayes, I. L., Smith, M. M., Sherry, S. B., Vidovic, V., Saklofske, D. H. (2019). Are perfectionism dimensions risk factors for bulimic symptoms? A meta-analysis of longitudinal studies. Personality and Individual Differences. doi: 10.1016/j.paid.2018.09.022
Le Grange, D., Lock, J., Agras, W. S., Bryson, S. W., & Jo, B. (2015). Randomized Clinical Trial of Family-Based Treatment and Cognitive Behavioral Therapy for Adolescent Bulimia Nervosa. Journal of the American Academy of Child & Adolescent Psychiatry, 54(11), 886-894. doi: 10.1016/j.jaac.2015.08.008
© 2026 InsideOut
InsideOut acknowledges the tradition of custodianship and law of the Country on which the University of Sydney and Charles Perkins Centre campus stands. We pay our respects to those who have cared and continue to care for Country. We are committed to diversifying research and eliminating inequities and discrimination in healthcare. We welcome all people regardless of age, gender, race, size, sexuality, language, socioeconomic status, location or ability.