Last Reviewed: 01 Jan 2022
Binge Eating Disorder (BED) is a type of eating disorder characterised by recurrent episodes of binge eating. A binge is defined as eating an unusually large amount of food in a short period of time. While eating, the person has a sense of lack of control.
To meet diagnostic criteria the binge eating episodes occur at least once a week for three months and are not followed by compensatory behaviours (American Psychiatric Association, 2022)
Binge eating episodes are associated with three (or more) of the following:
Eating much more rapidly than normal
Eating until feeling uncomfortably full
Eating large amounts of food when not feeling physically hungry
Eating alone because of feeling embarrassed by how much one is eating
Feeling disgusted with oneself, depressed, or very guilty afterward
Binges often occur in response to emotions, rather than hunger. Binge eating can be a way of coping with underlying personal and emotional difficulties, including boredom, loneliness, and anxiety. BED can be experienced by the individual as helping them to function by numbing their emotions, being a distraction from what is going on in their lives. Binges are followed by feelings of guilt, shame, disgust, and depression.
Binge eating can also be triggered by concerns around food, weight, and shape. For example, an individual may binge due to hunger or feeling deprived when dieting; or feelings of guilt when they feel they have eaten too much or broken a ‘diet rule’ and so they may as well keep going as they have ‘ruined’ things anyway.
Often individuals can get stuck in a cycle of bingeing. Two common cycles are detailed below:
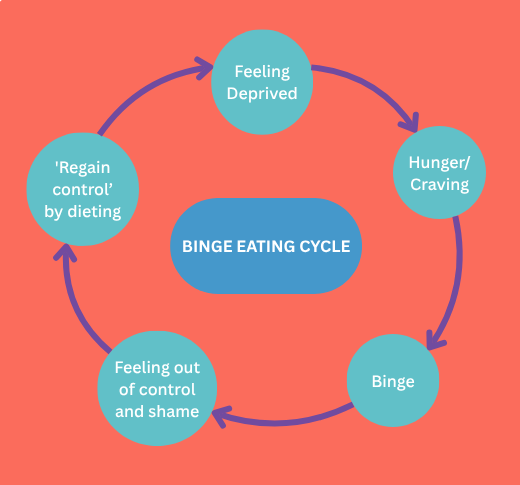
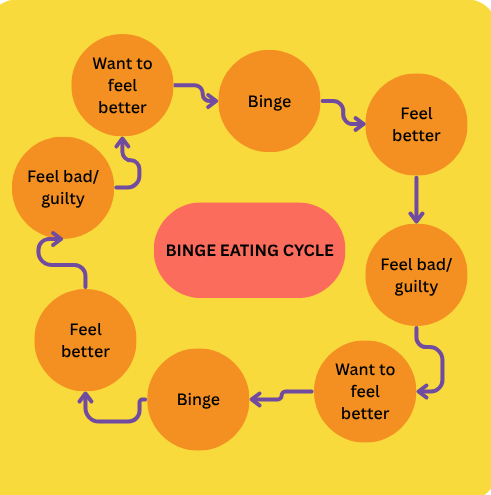
Between 1.1% and 3.7% of Australians will have BED in their lifetime.
Changes in weight
Feeling tired and not sleeping well
Feeling bloated or constipated
Preoccupation with eating, food, body shape and weight
Feelings of extreme distress, sadness, anxiety, and guilt during and after a binge episode
Low self-esteem
Increased sensitivity to comments relating to food, weight, body shape and exercise
Depression, anxiety, or irritability
Evidence of regular episodes of eating large amounts of food
Secretive behaviour relating to food
Avoiding eating with others
Evading questions about eating and weight
Increased isolation and withdrawal from activities previously enjoyed
Erratic behaviour (e.g., shoplifting food or spending large amounts of money on food)
Decreased ability to function in everyday life, including relationships, socialising, work, school, or recreational activities
Research suggests that a range of psychological therapies such as Cognitive Behavioural Therapy (CBT), Dialectical Behavioural Therapy (DBT), and Interpersonal Therapy (IPT) are most effective. Ongoing medical monitoring by a GP and nutrition support with a Dietitian is also important. For adults, CBT has been shown to be the most effective for treatment of BED.
‘Guided self-help’ has also been shown to be effective. BEeT is a free, online CBT program to reduce binge eating behaviours and support you with the associated thoughts and feelings.
For children and adolescents, both Family Based Treatment (FBT), CBT, DBT and IPT have some research to support their use in BED, although research is lacking in this area.
Hospital-based treatment may be required if the symptoms are very severe or if there are any medical complications that may need immediate treatment. For any individual with BED, it is important to seek care from an empathetic and skilled GP who can remain involved in care throughout treatment to monitor physical health. A trained and skilled community clinician will almost always be needed to deliver evidence-based treatment.
Anyone experiencing this pattern of eating, no matter how infrequent, should seek timely treatment.
References
American Psychiatric Association. (2022). Diagnostic and statistical manual of mental disorders (5th ed. Text Revision). Washington, DC: American Psychiatric Press.
Bohon, C. (2019). Binge Eating Disorder in Children and Adolescents, Child and Adolescent Psychiatric Clinics of North America, 28(4), 549-555. doi: 10.1016/j.chc.2019.05.003
Hudson JI, Hiripi E, Pope HG, Kessler RC. The Prevalence and Correlates of Eating Disorders in the National Comorbidity Survey Replication. Biological Psychiatry. 2007;61(3):348-358. doi:10.1016/j.biopsych.2006.03.040
Iacovino, J. M., Gredysa, D. M., Altman, M., & Wilfley, D. E. (2012). Psychological Treatments for Binge Eating Disorder, Current Psychiatry Reports. 14(4), 432-446. doi: 10.1007/s11920-012-0277-8
© 2026 InsideOut
InsideOut acknowledges the tradition of custodianship and law of the Country on which the University of Sydney and Charles Perkins Centre campus stands. We pay our respects to those who have cared and continue to care for Country. We are committed to diversifying research and eliminating inequities and discrimination in healthcare. We welcome all people regardless of age, gender, race, size, sexuality, language, socioeconomic status, location or ability.